
: Admin : 2021-12-23
What causes common clinical conditions of the spinal column?
The human body functions through an organised, structured organ system. Each organ system functions independently yet in an integrated manner to carry on different activities or functions within the body. The nervous system formed of the spinal cord, brain and bundle of nerves that spread throughout the body, performs voluntary and involuntary actions of the body. The nervous system carries impulses, receive information from the environment and generates responses to that information. It reacts to every external stimulus thereby helping all parts of the body to communicate or coordinate with each other.
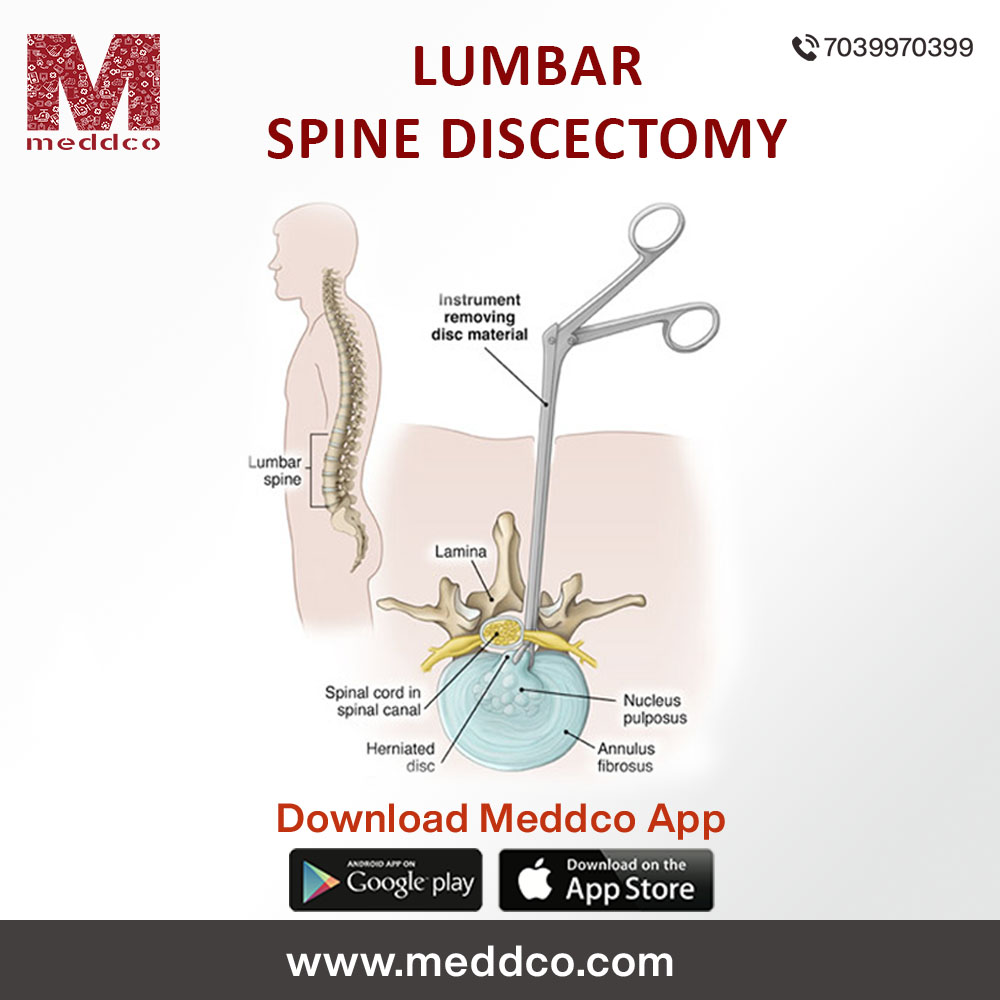
The spinal cord is protected by vertebral column. It is made up of bones that supports spinal cord from base of skull to the corda equina, a bunch of nerves in the back shaped like horse’s tail. A sequence of vertebra separated and united by intervertebral disc supports head, neck and body to control movements of the body. The lumbar spine at the back is formed of L1-- L5 vertebra that supports the lower part of spinal cord. The bones constituting the vertebral column protect spinal cord from injury. The intervertebral disc between each vertebra act as a cushion to the cord. Large nerves that originate from spinal cord emerge through a hole called foramen from the vertebral column. These nerve roots receive signals from the brain through the spinal cord to different parts of the body. Cervical spondylitis, lumbar spondylitis, disc prolapse are few diseases of the spinal cord. A degenerative change from old age or injury may weaken the outer wall of intervertebral disc. The soft, innner part of the disc bulge out due to degeneration, termed as herniated or bulging disc. The bulging disc compress the nerves of the spinal cord causing pain in surrounding parts of the body.
What is the treatment for lumbar spine disorders?
Patients with lumbar spine disease feels moderate continuous back pain, spasms, weakness with numbness in legs, calves or buttocks, abnormal gait and loss of sensation. X Ray, blood tests, MRI, electromyography and bone scans is done to find the location of pathology and cause of symptoms. A doctor asks the patient to stop all anti inflammatory drugs and blood thinners before 7 days. Once the diagnosis is confirmed treatment is decided by the orthopaedic surgeon. Medications and surgery are often the choice of treatment. Lumbar discectomy is a surgery done to remove herniated disc in the lower spine.
What is lumbar discectomy?
The herniated, bulging, prolapsed or slipped disc that constrict nerve fibres emerging from spinal cord cause unbearable pain. A lumbar disc is a surgery to cut or remove a herniated disc in lower back. It is considered a major surgery. When other treatment options fail while treating a ruptured disc, a doctor advices lumbar discectomy. Orthopaedic surgeons and neurosurgeons who are specialized in treating diseases of nervous system perform lumbar discectomy. The surgery is done using general anesthesia or regional anasthesia depending upon the procedure needed to be done for treating a patient suffering from herniated disc. It is done in a operation theater set up with all necessary medical apparatus.
How is lumbar discectomy done?
A complete medical history is recorded by the physician before the operation is scheduled. If a general anesthesia is required then a combination of intravenous medication and gases is given to the patient. A liquid anasthetic in the form of peripheral nerve block infusion is given at the site of surgery to control pain. A tube is placed within trachea to control breathing while patient is under general anesthesia. Regional anasthesia involves injecting anasthesia around certain nerves to make the area numb along with sedation that keeps the patient relaxed. A surgical team monitors patients vital signs and body functions during surgery.
The following methods are adopted by the surgeon. He chooses one of these procedures according to the pathological condition detected under scans and MRI.
OPEN SURGERY is done by making an incision upto 4 inch down the middle area of the affected spine. The doctor can directly visualize the area of the surgery. The ruptured disc is later removed with other procedures like laminectomy, foraminotomy and spinal fusion.
MICRODISCECTOMY is a minimal invasive surgical procedure. Special instruments are inserted through a narrow one inch diameter incision near the spinal area that is affected.
ANTERIOR DISCECTOMY is a procedure to remove the spinal disc by making an incision in the anterior part of the body.
PERCUTANEOUS AND ENDOSCOPIC DISCECTOMY is a minimal invasive surgical procedure is done using thin tubes with guide wires are placed through the tissues to disect herniated disc with minimal damage to surrounding areas.
The surgeon reaches the damaged disc through the posterior part of spine through the muscles and bones. The surgeon visualizes the disc by removing a portion of the lamina. Lamina is the bone that forms the roof of the spinal cord. Then the spinal nerve that gets compressed from the bulging disc is retracted on one side. A single disc or multiple disc that shows degenerative changes is later removed during the procedure. The muscle and skin incisions are stapled back and incision is sutured.
The lumbar discectomy is a common surgical procedure adopted by orthopaedic surgeon and neurosurgeons worldwide, to treat disc herniation.
What steps should patient follow post surgery?
A patient is allowed to move once the effect of anesthesia decreases. He is given pain killers and all his vital signs are monitored. He is discharged from the hospital within two days.
The patient is advised to avoid bending or twisting movements. He should not lift heavy weights nor do strenuous activity like house work. He is advised to stop driving and avoid alcohol consumption while on analgesics. Incision should be taken care of by applying ice packs. During follow-up visits the doctor will remove staples and stitches. Patients can resume work after a months rest.
He can prevent future episodes of back pain by taking necessary precautions.
He should completely avoid heavy weight lifting or use proper techniques while lifting during unavoidable circumstances. He should maintain relaxed, comfortable posture while sitting, standing and sleeping. He should maintain a mild exercise program and relaxation activities to be followed as a routine regime to manage stress. Smoking and alcohol consumption should be stopped.
What are the benefits or results of lumbar discectomy?
Patients with disc bulge or herniated disc get 90% relief from symptoms when treated through lumbar discectomy. It is a most advanced technique to a quick recovery of patients who suffer from back pain from a ruptured disc. It involves less blood loss, muscle trauma and faster recovery.
What are the possible risks and complications of lumbar discectomy?
Patients have the risk to infections, bleeding and injury to the covering of the spinal cord or injury to nerves, arteries or veins. The fragments of the herniated disc may cause pain, weakness and problems during urination.
The complications can be avoided through regular follow up sessions. Patients should be made aware about a specific health care regime.
The spinal cord disorders have been a cause of malaise in old age group and adults who perform heavy strenuous activity. The burden, pressure from load or weight rests primarily on shoulders and back. Vertebral column or back bone acts as a fulcrum, an axis supporting the most vital structure, the spinal cord. The degenerative diseases of spine are caused due rash, unhealthy traits or trauma from occupational activities. The damage or disc bulge either from degeneration or rupture can be treated through the traditional lumbar discectomy method or as a minimal invasive surgery. In both the methods patients get relief from lower back pain.
What physical therapy is advised post lumbar discectomy?
A patient who has a lumbar disc prolapse, has to undergo surgical treatment procedure if the pathology is deep rooted or is advised to follow physical therapy sessions if he complains of mild or moderate intensity pain with symptoms like weakness and numbness.
A physical therapy is also recommended to patients post surgery to avoid complications and help in speedy recovery. A physical therapy helps patient to strengthen posture, muscles and prevent pressure on spinal nerves.
PRONE EXTENSION – Patients should lie in prone position on stomach, propping and exercising on the elbows. Patient should hold on to this position for five minutes. This method can be made more advanced by moving upper body off the ground with your hands. A patient should continue upto 5 sets daily.
DYING BUG – Patient has to lie down with knees bent and feet touching the floor. The abdominal muscles should contract and back rested on the ground. Place your legs off the ground, slowly start marching back and down one at a time. Lift your arms alternalty overhead and back of your side.
STANDING ROW – While doing this exercise, hold each of band on your hand while other end should be tied with the strong support. A patient should squeeze on the shoulders as you pull the band backwards with both the hands. The neck should be kept erect while no strain on back only by movements of arms and shoulders exercise can be done upto three sets of 10 repetitions.
In BIRD DOG exercise—a patient bends on hands and knees. The abdominal muscles will squeeze so low back would rest like a flat like a table top. The patient should gradually extend the opposite leg by alllowing the pelvis to tilt and raise one arm over the head. Patients should hold on this position for 10 seconds and repeat upto 3 sets of 10 repetitions daily. Aerobic and core strengthening exercises are also advised by the physician.
An integrated approach through exercises without lifting heavy weights but performing physical therapies that make tissues and muscles surrounding the bones strong should be done post surgery to maintain a healthy life.
lumbar spine spinal cord
No Comments